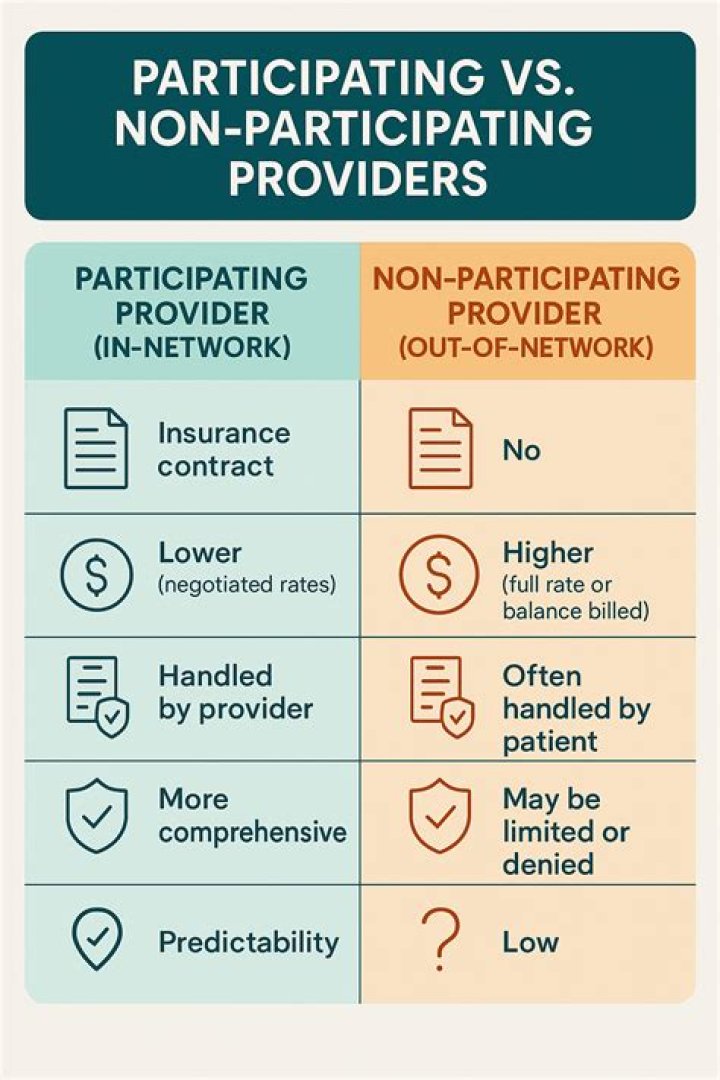
– A participating provider is one who voluntarily and in advance enters into an agreement in writing to provide all covered services for all Medicare Part B beneficiaries on an assigned basis. – A non-participating provider has not entered into an agreement to accept assignment on all Medicare claims.
What is the difference between preferred and participating providers?
A provider who has a contract with your health insurer or plan to provide services to you at a discount. Participating providers also contract with your health insurer or plan, but the discount may not be as great, and you may have to pay more. …
What is a non-participating physician?
A nonparticipating provider is a provider involved in the Medicare program who has enrolled to be a Medicare provider but chooses to receive payment in a different method and amount than Medicare providers classified as participating.
What are the advantages of a member seeing a participating provider instead of a non-participating one?
The advantages of being a participating provider: Higher allowances (5% higher than non-participating providers). Direct payment (Medicare sends payment directly to the provider, not the patient). Medigap transfer (Medicare forwards claims on to Medigap insurers for providers).
What is a participating physician?
Participating Physician means a Physician who, at the time of providing or authorizing services to a Member, is under contract to provide Professional Services to Members.
What is the definition of participating provider?
Participating Provider — a healthcare provider that has agreed to contract with an insurance company or managed care plan to provide eligible services to individuals covered by its plan. This provider must agree to accept the insurance company or plan agreed payment schedule as payment in full less any co-payment.
What is a non preferred provider?
A provider who doesn’t have a contract with your health insurer or plan to provide services to you.
What are participating providers?
What is the difference between par and non par?
A ‘Par provider’ is a doctor who accepts assignment. A ‘Non-Par’ provider is a doctor who does not accept assignment. Typically, a Par Provider bills Medicare directly an amount equal to the Medicare ‘Par Fee’. The NonPar Fee is 5% less than the Par Fee.
What is participating and non-participating provider in medical billing?
Meaning. A participating policy enables you, as a policyholder, to share the profits of the insurance company. These profits are shared in the form of bonuses or dividends. It is also known as a with-profit policy. In non-participating policies, the profits are not shared and no dividends are paid to the policyholders.
What is the difference between non participating and participating providers?
Non-participating providers accept Medicare but do not agree to take assignment in all cases (they may on a case-by-case basis). This means that while non-participating providers have signed up to accept Medicare insurance, they do not accept Medicare’s approved amount for health care services as full payment.
What is the difference between Medicare participating and non-par?
All Medicare covered services must be billed to Medicare, or the provider could face penalties. A non-par provider is actually a provider involved in the Medicare program who has enrolled to be a Medicare provider but chooses to receive payment in a different method and amount than Medicare providers classified as participating.
What are participating providers and do they accept Medicare?
Participating providers accept Medicare and always . Taking means that the provider accepts Medicare’s for health care services as full payment. These providers are required to submit a bill (file a ) to Medicare for care you receive.
What is the Medicare limit for non participating providers?
Non-participating providers can charge up to 15% more than Medicare’s approved amount for the cost of services you receive (known as the limiting charge ). This means you are responsible for up to 35% (20% coinsurance + 15% limiting charge) of Medicare’s approved amount for covered services.